A monthly vaginal ring is one significant step closer to potentially becoming a new HIV prevention method for cisgender women in sub-Saharan Africa, who face persistently high rates of HIV infection but have few options to protect themselves. Story highlights work from Biostatistics researchers Elizabeth Brown and Barbra Richardson.
In the News




A new study finds that the use of estrogen alone among women who had a prior hysterectomy resulted in a lower rate of breast cancer incidence and mortality. UW Biostatistics faculty members and Fred Hutch researchers Ross Prentice and Garnet Anderson are among the study co-authors.
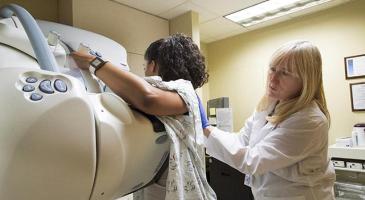
“This study incorporated so much data and from sites that are geographically, racially, and ethnically diverse, and this allowed us to explore questions that other researchers have not,” — Study co-lead author R. Yates Coley (PhD ’14), affiliate assistant professor of biostatistics and an investigator at Kaiser Permanente Washington Health Research Institute

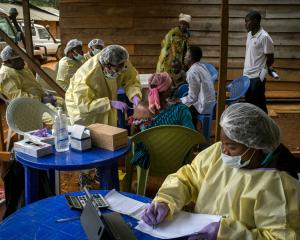
“There are risk predictors that account for space and geography and features that are more constant like race, ethnicity or preexisting conditions. It’s really complicated," says Research Professor of Biostatistics Peter Gilbert.


Thomas Fleming, professor of biostatistics, co-authored a recently published JAMA paper that addresses issues important to protecting the integrity of clinical trials conducted during the COVID-19 pandemic.
UW Biostatistics faculty members Thomas Fleming and Betz Halloran are among five leading biostatisticians and epidemiologists who debate the probable scope and duration of the pandemic, the kinds of medical responses that we need, and some of the impacts they foresee on the U.S. and on the world. They also discuss the pandemic's likely effect on higher education.

Betz Halloran, professor of biostatistics and director of the Center for Inference and Dynamics of Infectious Diseases at Fred Hutchinson Cancer Research Center, is featured in this recent PBS News story. “You can't believe every number that comes out. But if we don't try to formulate our thinking about a complex process, then we will be running blind,” says Halloran.


Xihong Lin (PhD, ’94), professor and former chair of the Department of Biostatistics and professor of statistics at Harvard University, gave a talk about data surrounding public health interventions that were put into place in Wuhan, China, which she compared to interventions implemented in the United States and in various countries in Europe. Watch the recorded presentation and read the take-home messages.